A patient applies a patch. The expectation is simple: it stays on, it delivers its medicine, and it comes off cleanly. This simple act, however, relies on a profound engineering paradox.
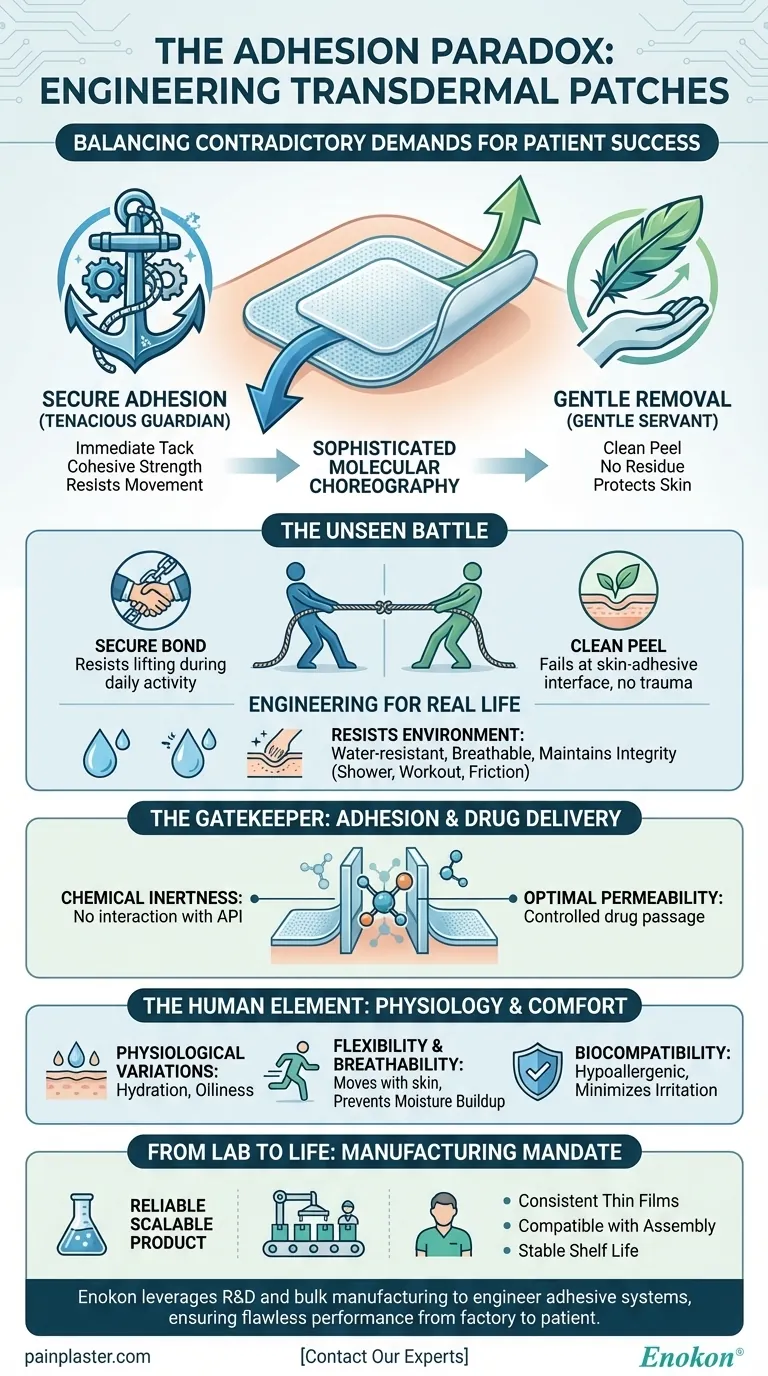
The adhesive on that patch must be two contradictory things at once. It must be a tenacious guardian, holding fast through sweat, showers, and the friction of daily life. Yet, days later, it must become a gentle servant, peeling away without damaging the skin or leaving a trace.
This is the silent contract between the patch and the patient. Fulfilling it requires a deep understanding of material science, pharmacology, and human physiology. It's less about simple "stickiness" and more about sophisticated molecular choreography.
The Unseen Battle: Secure Adhesion vs. Gentle Removal
The primary conflict lies in balancing adhesion with removal. An effective adhesive must form a secure, continuous bond with the skin to ensure the drug can be delivered consistently.
- Secure Adhesion: This is achieved through a combination of initial "tack" (the immediate stickiness) and cohesive strength (the internal integrity of the adhesive). It has to resist lifting at the edges as the body moves and flexes for days on end.
- Gentle Removal: The bond must be strong, but not too strong. Upon removal, the adhesive should fail at the skin-adhesive interface, not within the adhesive itself (leaving residue) or by stripping away layers of the stratum corneum (causing skin trauma).
Achieving this perfect balance is a masterclass in polymer engineering, tuning the formulation to release its grip when needed.
Engineering for Real Life: Resisting the Environment
A patient’s life doesn’t pause for a patch. The adhesive must be engineered for the real world—a world of varying humidity, temperature, and physical stress.
It must maintain its integrity during a hot shower, a sweaty workout, or simply under the constant friction of clothing and bedding. This often involves incorporating specialized polymers that are water-resistant yet breathable, preventing the skin from becoming macerated underneath.
The Gatekeeper: Balancing Adhesion and Drug Delivery
The adhesive is not just a physical anchor; it is an active participant in the drug delivery system. It serves as the gatekeeper between the drug reservoir and the skin.
This creates another set of demands:
- Chemical Inertness: The adhesive cannot react with or degrade the active pharmaceutical ingredient (API).
- Optimal Permeability: It must allow the drug molecules to pass through it at a precise, controlled rate. The adhesive’s properties must be perfectly matched to the drug’s molecular weight and solubility.
If the adhesive is too impermeable, the therapy fails. If it interacts with the drug, the dose may be compromised. Therefore, the adhesive formulation is as critical as the drug itself.
The Human Element: Physiology and Comfort
Skin is not a uniform, inert surface. It is a living, breathing organ that varies dramatically from person to person and even across different locations on the same body. An adhesive must account for:
- Physiological Variations: Skin hydration, oiliness, and natural exfoliation rates all impact adhesion.
- Flexibility & Breathability: The patch must move with the skin without causing irritation. Breathability is key to preventing moisture buildup and ensuring long-term comfort.
- Biocompatibility: The materials must be hypoallergenic to minimize the risk of sensitization or allergic reactions.
Patient compliance hinges on comfort. If a patch is irritating, inflexible, or painful to remove, a patient is far less likely to use it as prescribed.
From Lab to Life: The Manufacturing Mandate
All this sophisticated science is meaningless if it cannot be translated into a reliable, scalable product. The adhesive must not only perform on the skin but also on the production line. It needs to be processable into consistent, high-quality thin films, maintain its properties throughout its shelf life, and be compatible with complex drug-loading and patch-assembly processes.
This is where technical expertise in formulation and manufacturing becomes non-negotiable. Turning a precise chemical formula into millions of identical, effective, and safe transdermal patches is the final, crucial step in solving the adhesion paradox. At Enokon, we leverage our deep R&D and bulk manufacturing capabilities to engineer adhesive systems that meet these competing demands, ensuring your therapeutic product performs flawlessly from the factory to the patient.
If you are navigating these complex challenges for your transdermal product, our expertise can provide the solution. Contact Our Experts
Visual Guide
Related Products
- Far Infrared Heat Pain Relief Patches Transdermal Patches
- Silicone Scar Sheets Patch Transdermal Drug Patch
- Icy Hot Menthol Medicine Pain Relief Patch
- Menthol Gel Pain Relief Patch
- Mugwort Wormwood Pain Relief Patch for Neck Pain
Related Articles
- Beyond Removal: The Hidden Pharmacokinetics of Transdermal Patches
- The Silent Workhorse: How Transdermal Patches Rewrote the Rules of Pain Management
- Beyond the Pill: The Engineering That Liberates Patients from Digestive Side Effects
- Engineering Certainty: The Invisible Architecture of a Gold-Standard Clinical Trial
- Beyond the Pill: The Physics and Psychology of Transdermal Pain Relief